Award-Winning Smiles for 45 Years
Boger Dental, the top office in Plymouth, is here to help you feel confident in your smile. We care for every kind of dental need, including cosmetic, restorative, and general dentistry.
Patient Center
 Watch Video
Watch Video
Cosmetic and Family Dentistry
Our award-winning team is committed to enhancing your lives and helping you to have the best smiles in our community!
Modern Dental Services
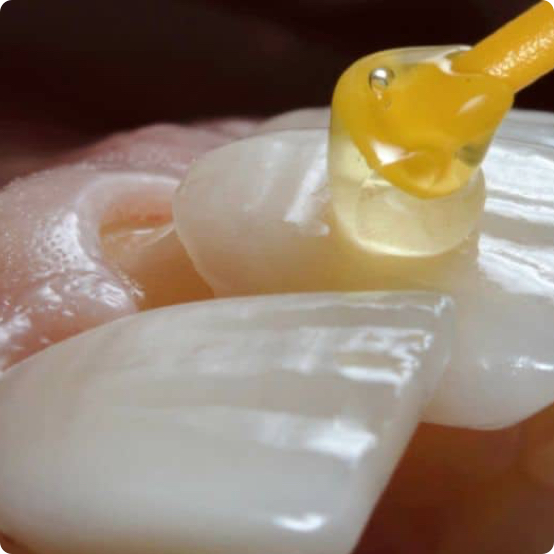
Veneers
Whether you have worn teeth or stained teeth, our veneers can help you achieve a more beautiful you.
Learn More
Teeth Whitening
Having a bright smile can do wonders for your confidence and self-esteem. See us to whiten your teeth at our Plymouth office.
Learn More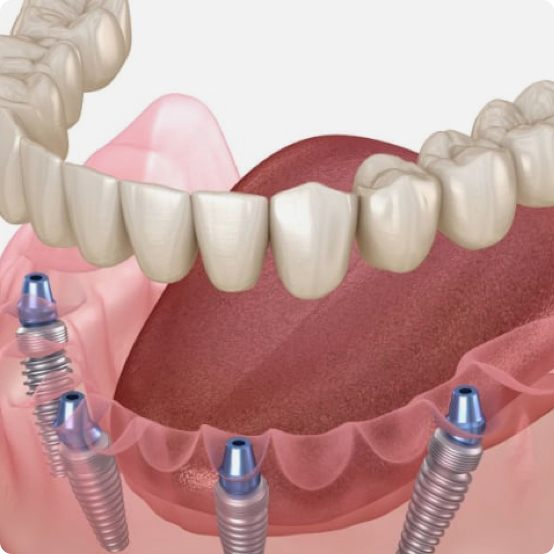
Dental Implants
Many people choose dental implants because they provide a high-quality, lasting solution to missing teeth.
Learn More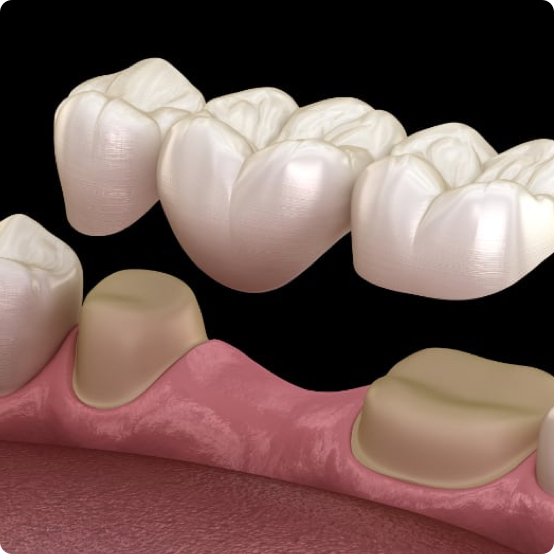
Dental Bridges
A bridge “bridges” the space between two teeth using a dental appliance that replaces one or more natural missing teeth.
Learn More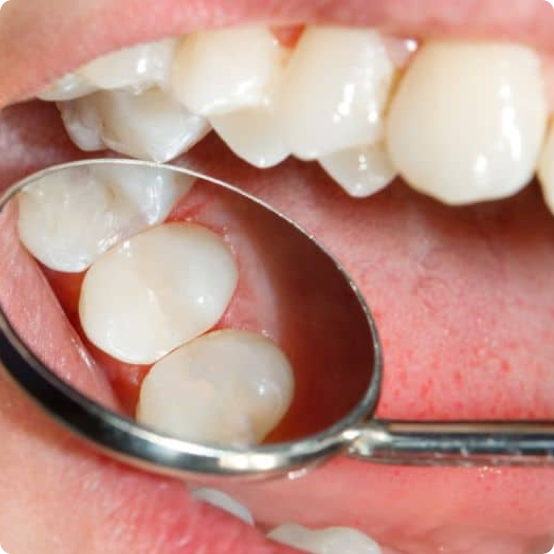
Tooth-Colored Fillings
Stop tooth decay without obvious silver fillings. Tooth-colored fillings can be used anywhere in your mouth.
Learn More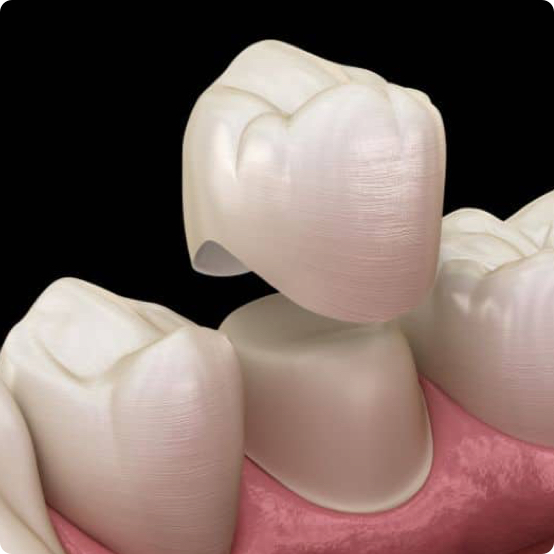
Dental Crowns
Our high-quality prosthetic crowns and bridges are made from porcelain, zirconia, gold, porcelain fused to metal, and ceramic crowns.
Learn More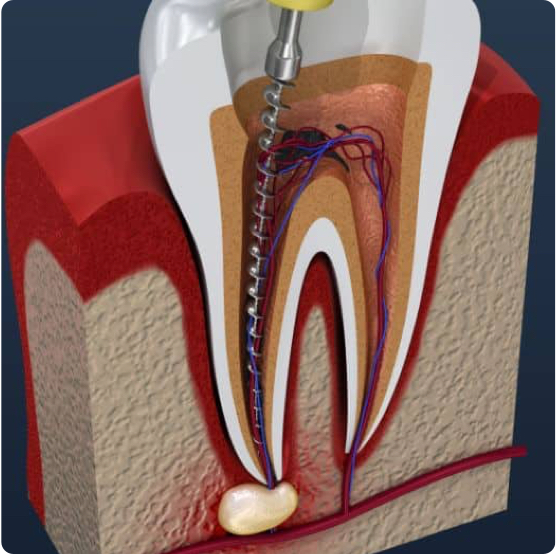
Root Canals
A root canal is a procedure used to save a badly decayed or damaged tooth, to prevent an infection or abscess.
Learn More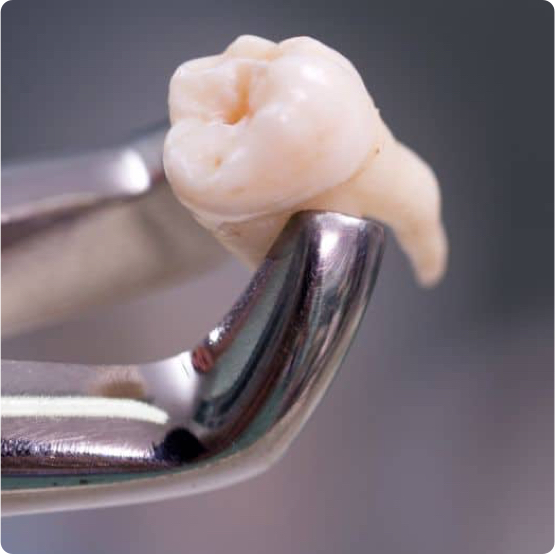
Tooth Extractions
We have performed hundreds of successful extractions for those with severe pain, damage, impacted teeth, or infected teeth.
Learn More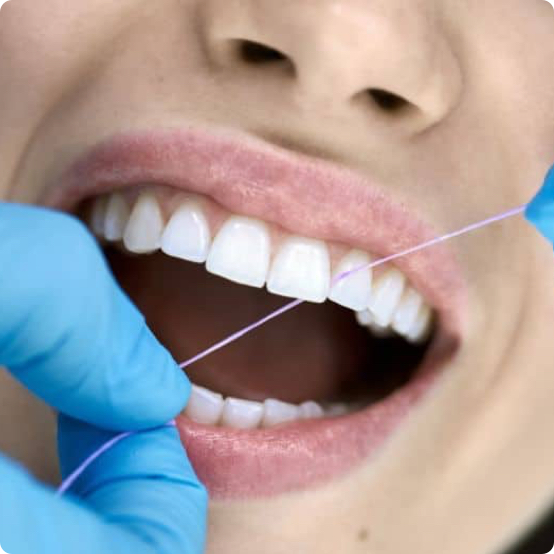
Preventative Cleanings
We provide comprehensive checkups to assess your overall oral health and recommend appropriate treatments for dental concerns.
Learn More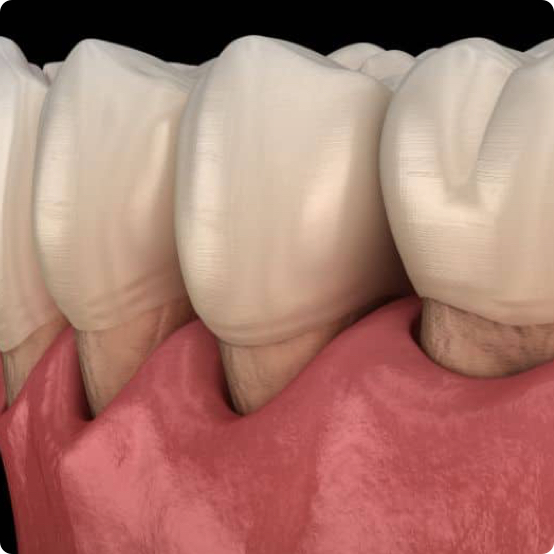
Gum Disease Treatment
If your at-home care is lacking and you miss your regular cleanings, you’re at an increased risk of developing gum disease.
Learn More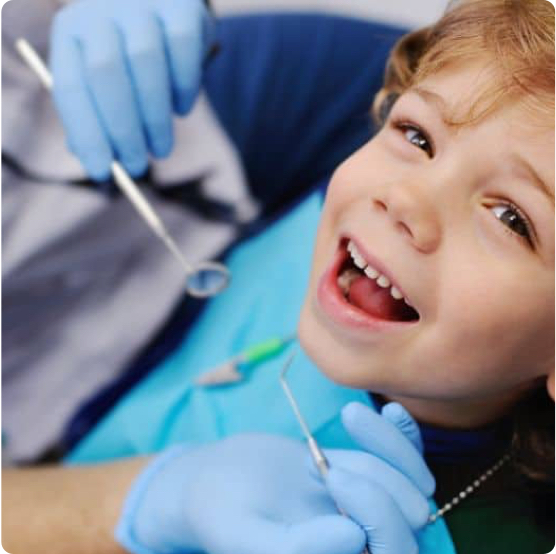
Children's Dentistry
The Boger Dental team is proud to offer a variety of pediatric dentistry services to help your child smile brightly for years to come.
Learn More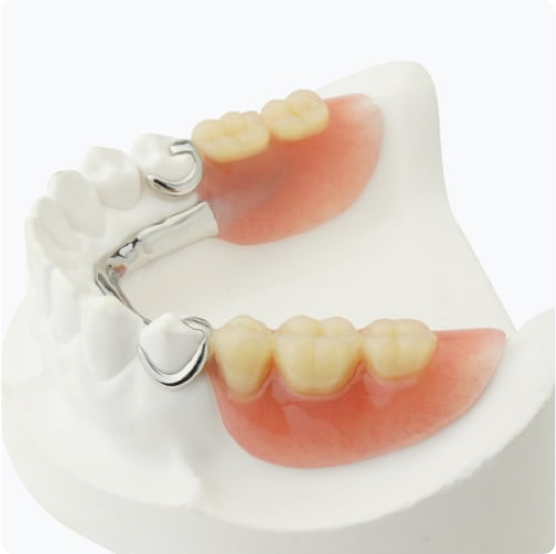
Removable Partial Dentures
Patients choose partial dentures for their flexibility, comfort, and natural appearance, and appreciate them as a non-invasive option.
Learn More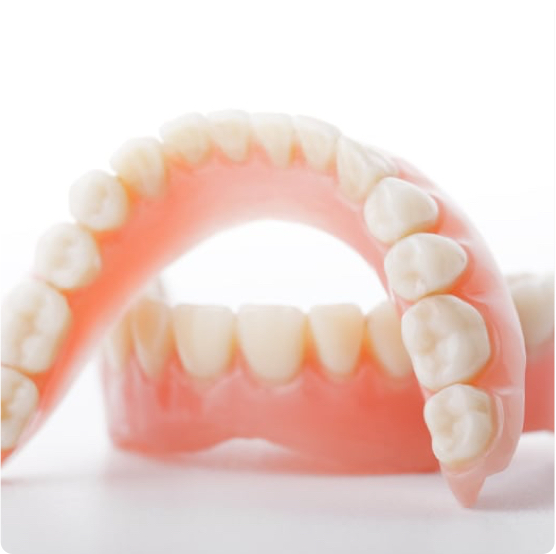
Dentures
You want your smile back, and dentures from Boger Dental can help make that happen. We offer high-quality, natural looking dentures.
Learn More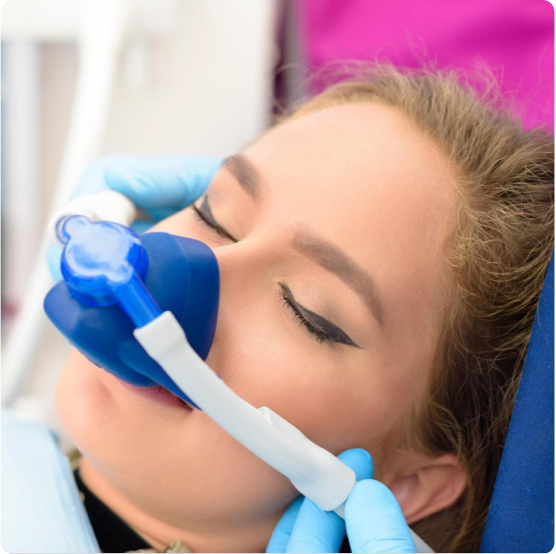
Sedation Dentistry
If you feel anxious about going to the dentist, you have new treatment options at Boger Dental to help you.
Learn More-
It's clear customer service is a top priority for everyone at Boger Dental. I didn't think I would ever describe a dentist's office as classy, but this place feels like a luxury experience.
- Rachel S. -
-
It's clear customer service is a top priority for everyone at Boger Dental. I didn't think I would ever describe a dentist's office as classy, but this place feels like a luxury experience.
- Rachel S. -
-
It's clear customer service is a top priority for everyone at Boger Dental. I didn't think I would ever describe a dentist's office as classy, but this place feels like a luxury experience.
- Rachel S. -

 Watch Video
Watch Video
Lisa
“As a person with high anxiety with dental care, all of these behaviors bring me back time and time again. Thank you for your care, your concern, and especially, your awesome team!!”
View AllShanthini
“Dr. Chad Boger is a wonderful dentist! I had a semi-emergency and he got me in right away the same day. He actually came back to work after he had left for the day just to help me.”
View All
 Watch Video
Watch Video


No Insurance?
No problem!
Take advantage of Smile Savings, Boger Dental’s exclusive dental savings program. Save big on full-service care for your whole family without the hassles and limitations of traditional insurance.
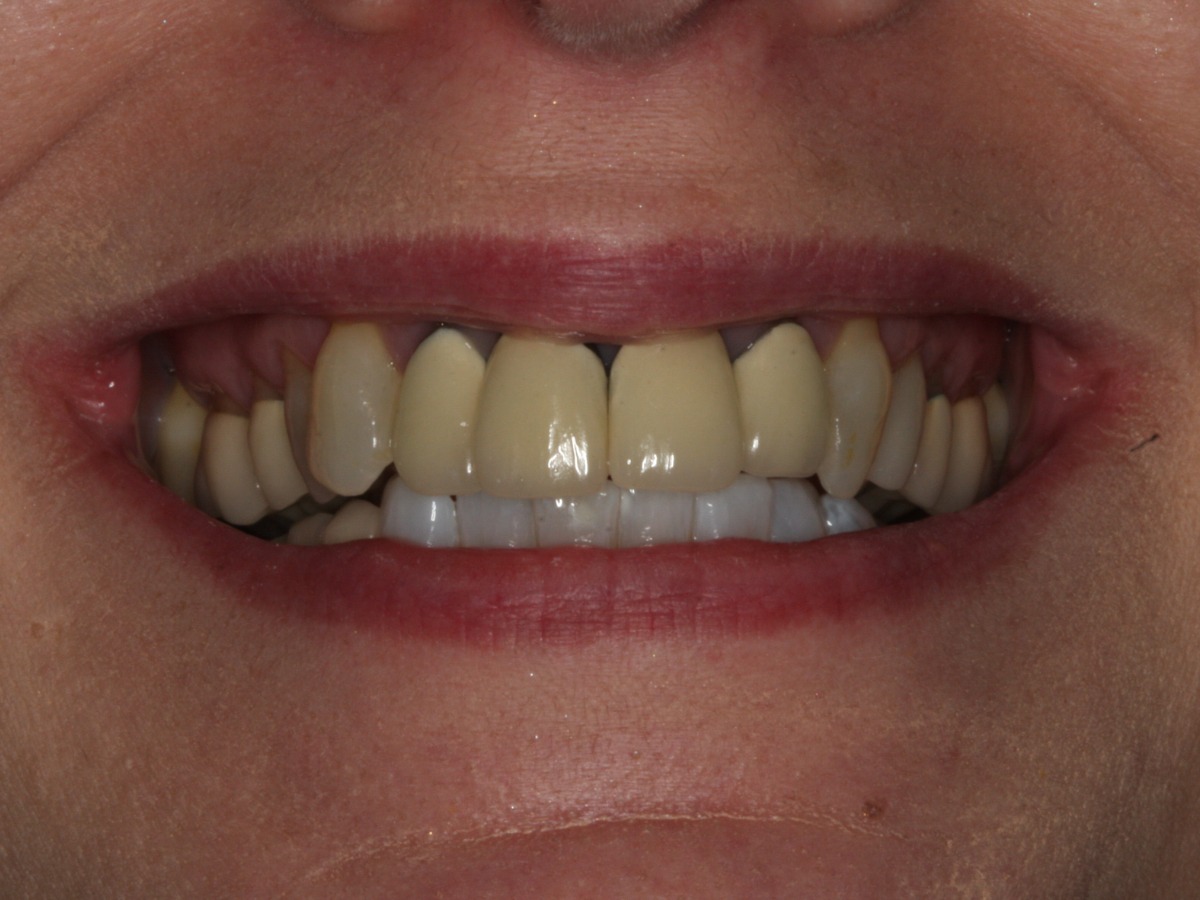
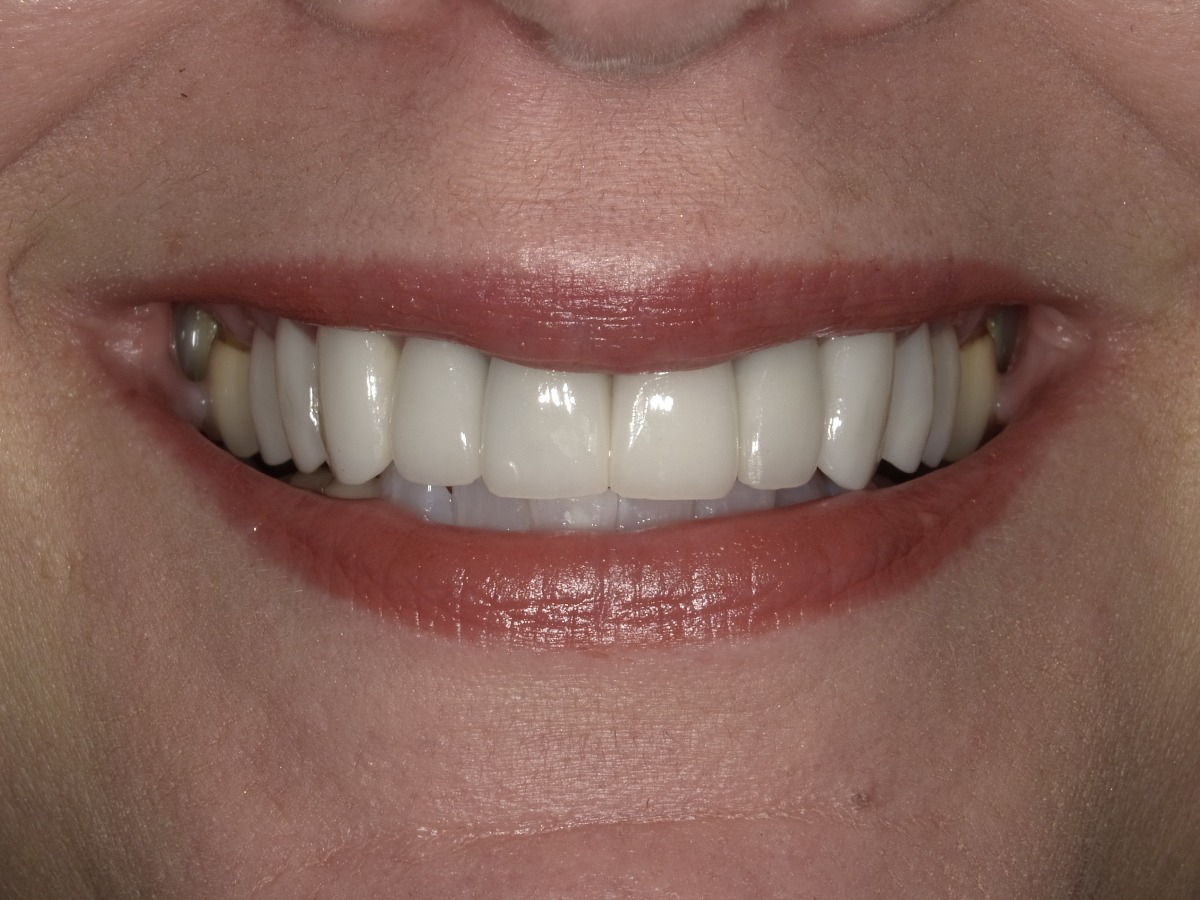
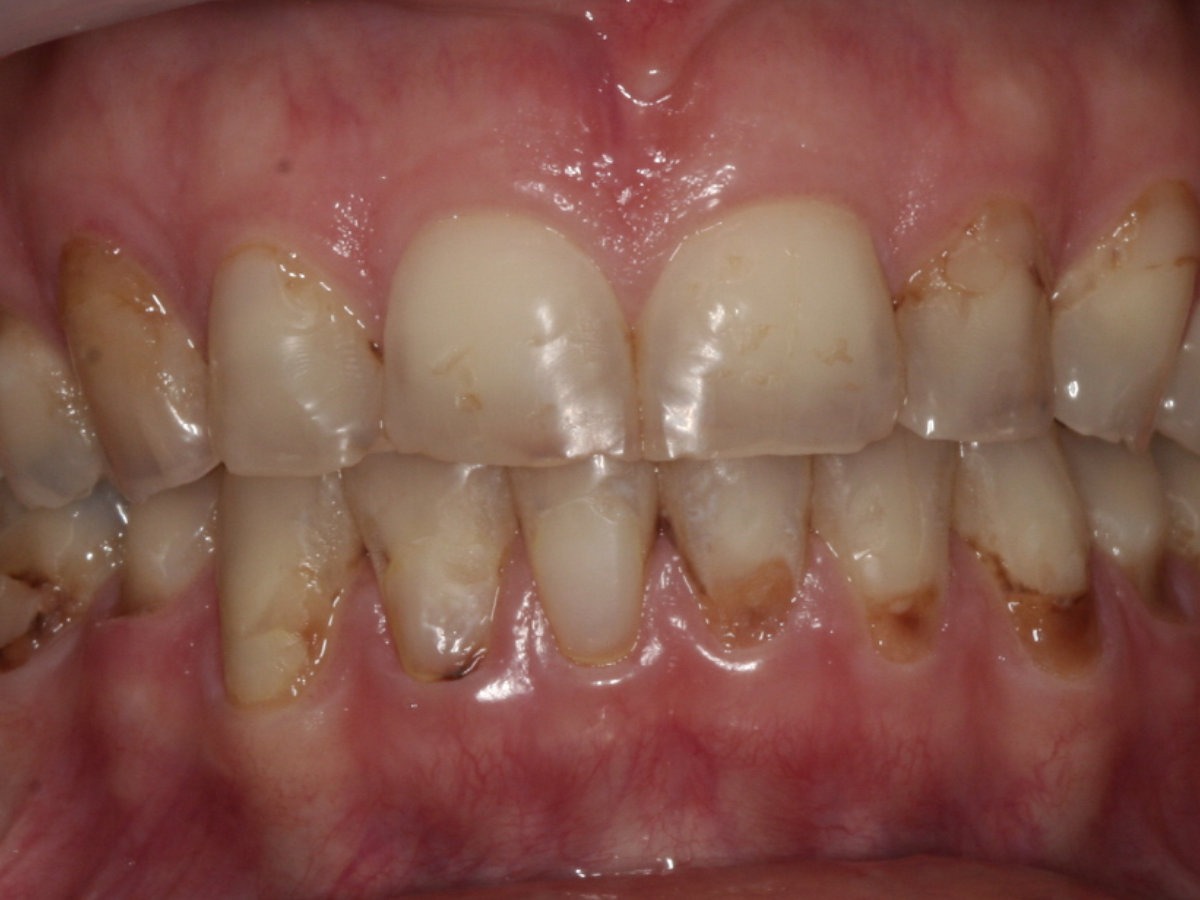
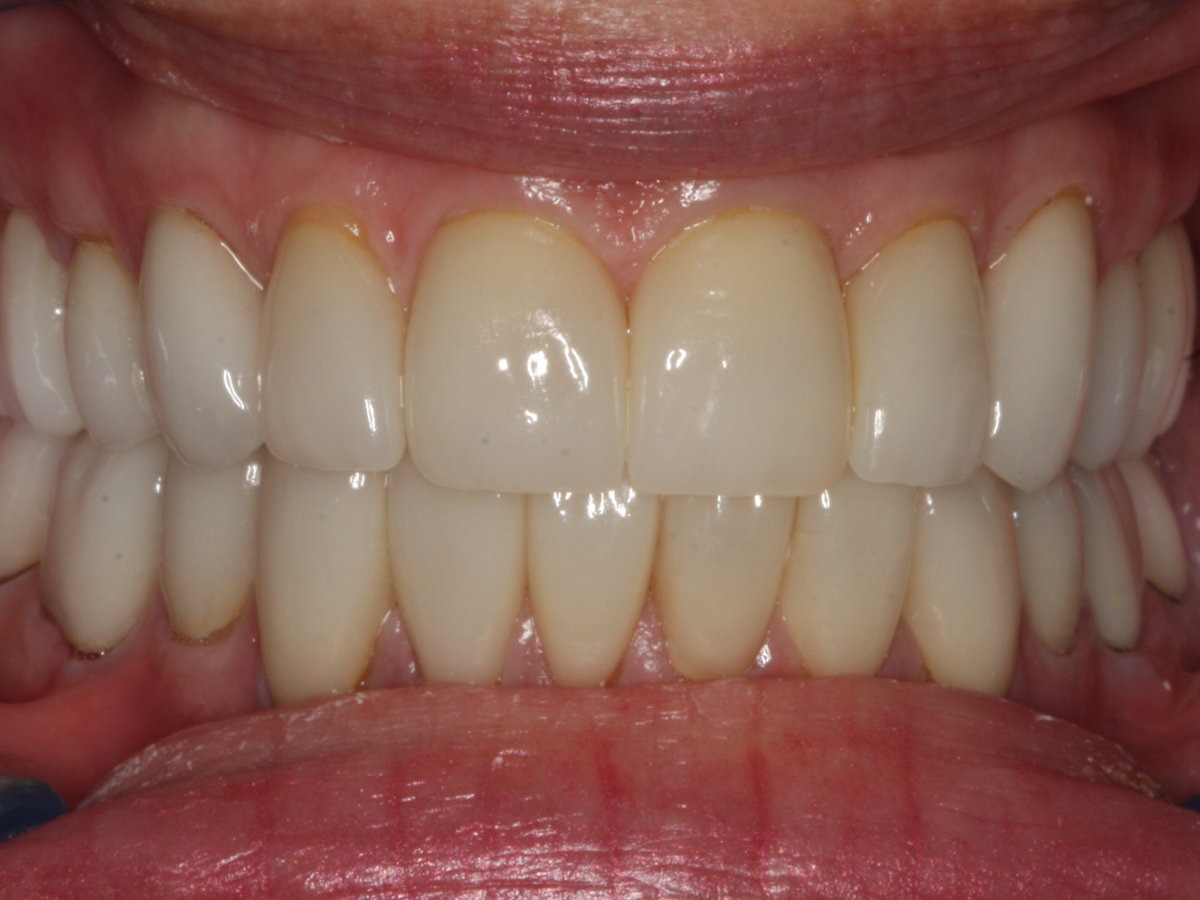
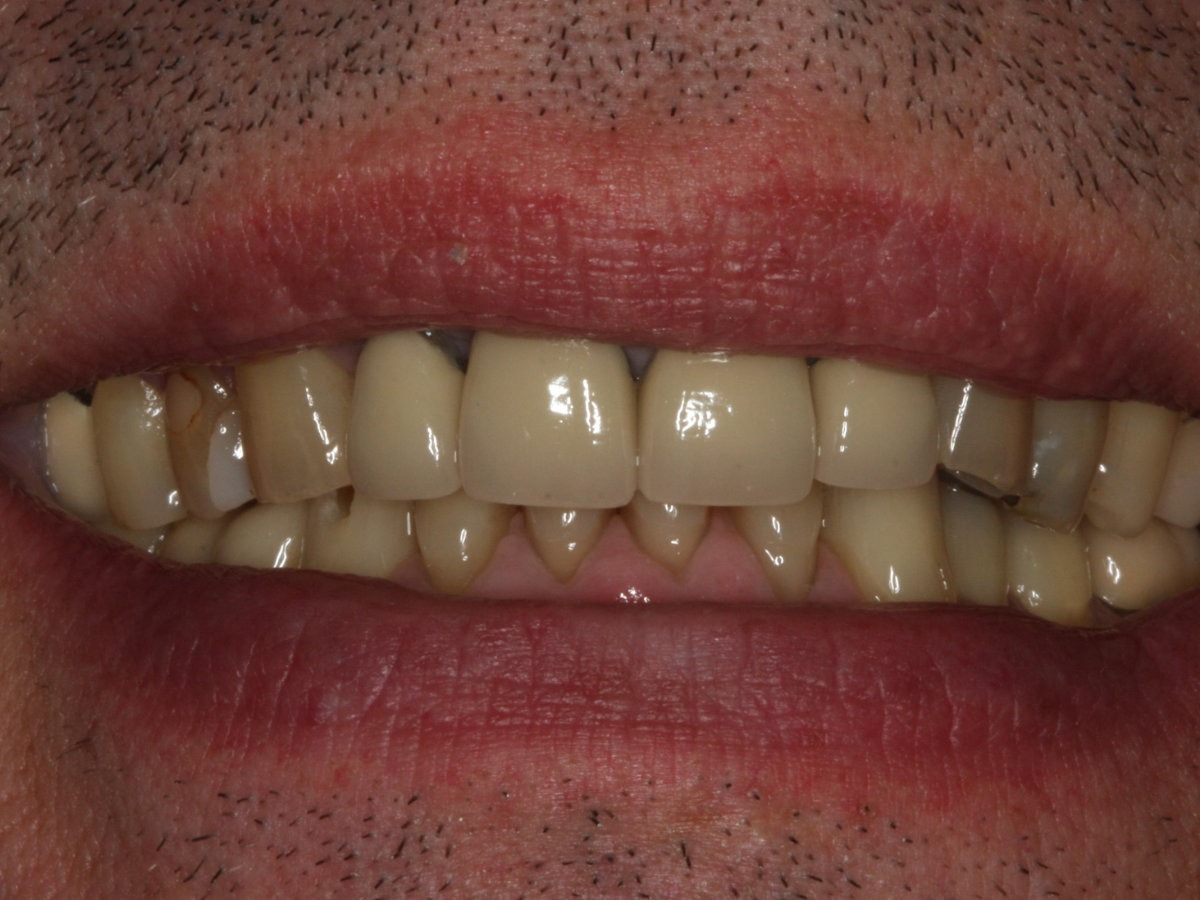
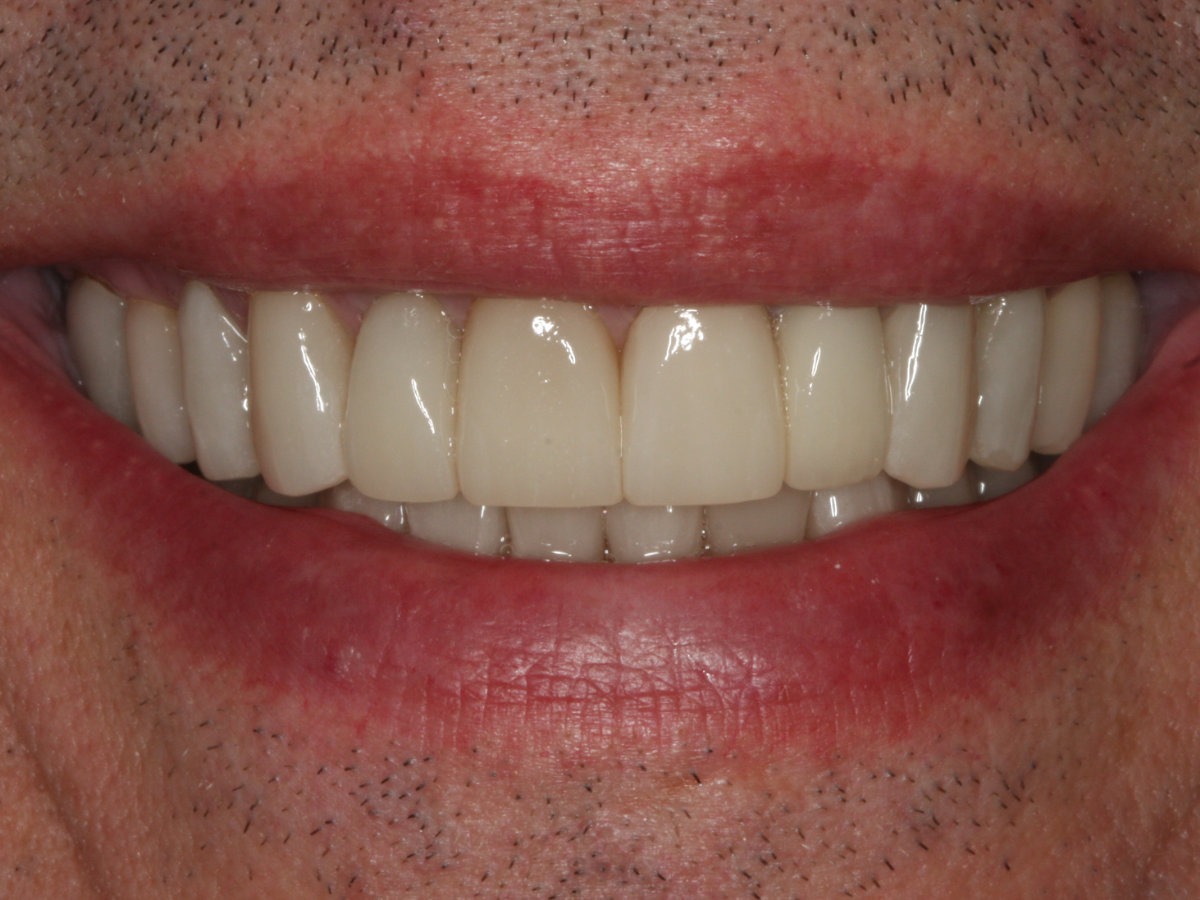
Learn MoreBefore & After Comparison
If you’re ready to smile without feeling self-conscious, confidently speak in public, and restore a younger smile, we can help!
View AllSchedule Your Appointment
Join thousands of patients around Plymouth who have transformed their smiles through our cosmetic and restorative dental treatments.